|
 |
- Search
| Obstet Gynecol Sci > Volume 59(2); 2016 > Article |
Abstract
Objective
To update information on the clinical and microbiologic characteristics of pediatric vulvovaginitis in Korean prepubertal girls.
Methods
A total of 120 girls (aged 0 to 9 years) with culture-confirmed pediatric vulvovaginitis, diagnosed between 2009 and 2014, were enrolled in the study. The epidemiologic and microbiologic characteristics, and clinical outcomes were assessed. Patients with sexual precocity, as well as those who were referred for suspected sexual abuse, were excluded.
Results
Girls aged 4 to 6 years were at the highest risk of pediatric vulvovaginitis. Seasonal distribution indicated obvious peaks in summer and winter. Of the 120 subjects, specific pathogens were identified in the genital specimens in only 20 cases (16.7%). Streptococcus pyogenes (n=12, 60%) was the leading cause of specific vulvovaginitis. Haemophilus influenzae was isolated in one patient. No cases presented with enteric pathogens, such as Shigella or Yersinia. A history of recent upper respiratory tract infection, swimming, and bubble bath use was reported in 37.5%, 15.8%, and 10.0% of patients, respectively. Recent upper respiratory tract infection was not significantly correlated with the detection of respiratory pathogens in genital specimens (P>0.05). Of 104 patients who underwent perineal hygienic care, 80 (76.9%) showed improvement of symptoms without antibiotic treatment. Furthermore, the efficacy of hygienic care was not significantly different between patients with or without specific pathogens (P>0.05).
Inflammation of the vulvar and vaginal epithelium, vulvovaginitis, is frequently reported in prepubertal girls. Patients present with signs and symptoms such as vaginal discharge, redness of the vulva, and genital soreness. Archetypal low estrogen milieu, as well as a proclivity for deprived local hygiene, in young prepubertal girls are the main causes of susceptibility to non-specific pediatric vulvovaginitis [1,2]. In addition, bubble bath use, and a medical history of upper respiratory tract infection (URI) or vulvovaginitis have been reported as risk factors for pediatric vulvovaginitis [1,3].
In 25% to 75% of prepubertal girls with symptoms of vulvovaginitis, genital microbiologic investigations indicate the presence of normal vaginal microflora or non-pathogenic bacteria [4]. Specific pathogens are reported in <50% of patients, and are typically respiratory in origin [5,6,7,8]. Streptococcus pyogenes is the leading cause of specific pediatric vulvovaginitis [5,7].
Although there are numerous reports on the causative microorganisms and clinical features of pediatric vulvovaginitis, data from Korea is very limited. A solitary Korean study, published by our institute in 1999, described some clinical aspects of pediatric vulvovaginitis using data from a small number of cases [6]. In that study, Haemophilus influenzae had been reported as the most common pathogenic bacteria, unlike the results of western studies in recent years. The present study aimed to reinforce the information on clinical characteristics of pediatric vulvovaginitis in Korean prepubertal girls with data from participants of larger studies as well as to elucidate contemporary changes in microbiologic etiology since 1999.
This was a retrospective analysis of data from 120 prepubertal girls, aged 0 to 9 years, who presented to the outpatient clinic for pediatric and adolescent gynecology at the CHA Bundang Medical Center between January 2009 and December 2014. Cases were defined as prepubertal girls who visited a clinic with typical genital symptoms or physical findings consistent with vulvovaginitis, either vaginal discharge and/or genital redness. Children who were diagnosed without culture were excluded. Patients with a record of Tanner stage ≥2 for breast development were excluded from this study. In addition, patients who were referred to the clinic for the evaluation of genital trauma or child sexual abuse were also excluded.
Patient demographics, presenting symptoms, objective findings of external genitalia, and clinical outcomes were assessed. The patient history for URI in the previous month, bubble bath use, and swimming were analyzed as associated factors.
All subjects had undergone vaginal (n=108) or vulvar (n=12) swabs for culture of aerobic bacteria or yeasts using conventional culture methods. Vulvar swabs had been selectively performed in subjects with small hymenal opening inadequate for vaginal swab (n=8) or subjects with severe vulvar inflammation without vaginal discharge (n=4). The swabs were transported in Amies transport medium, and cultured on 5% sheep blood agar, chocolate agar, and MacConkey agar. Additionally, 7 subjects with abnormal hymenal configuration had undergone Chlamydia antigen polymerase chain reaction from genital specimens. An early morning cellophane tape test had been selectively performed on 10 subjects with genital pruritus to confirm the presence of pinworm eggs. No cases had undergone anaerobic culture tests. Among 6 cases presenting with urinary symptoms, 2 cases with moderate to severe urinary symptoms underwent further investigation by urine culture. In contrast, 4 cases with a definite finding of vaginal discharge accompanied with mild urinary symptoms did not undergo urine microbiologic study.
Subjects were routinely provided instructions for perineal hygienic care at their first visit. The instructions included use of frequent sitz baths, genital drying, and front-to-back wiping, along with avoidance of genital irritants and tight underpants. Treatment success was defined as the complete or partial improvement of genital symptoms without the requirement for antibiotics.
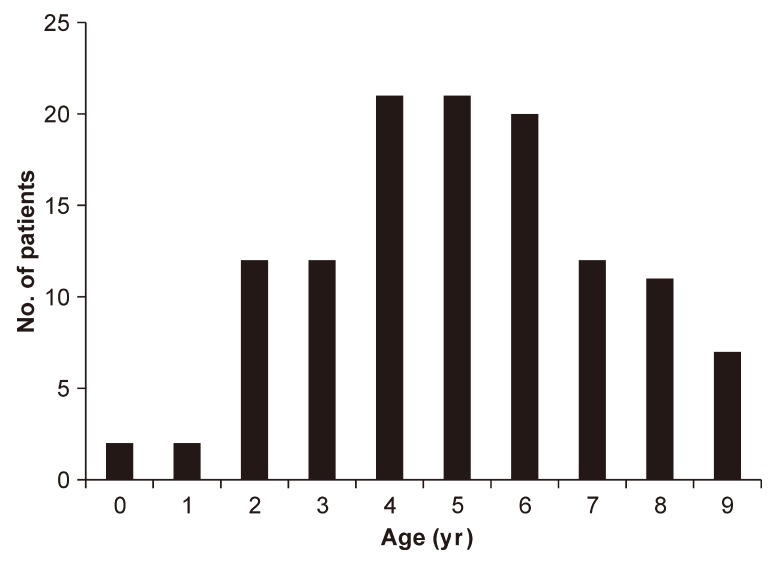
The age of the patients at presentation is illustrated in Fig. 1. The peak age at presentation was 4 to 6 years, and the mean (±standard deviation) age was 5.1 (±2.1) years. The seasonal distribution at presentation demonstrated an obvious bimodal trait with peaks in summer and winter (Fig. 2A). However, in terms of the time of symptom onset, the seasonal distribution represented a less apparent bimodal trait (Fig. 2B).
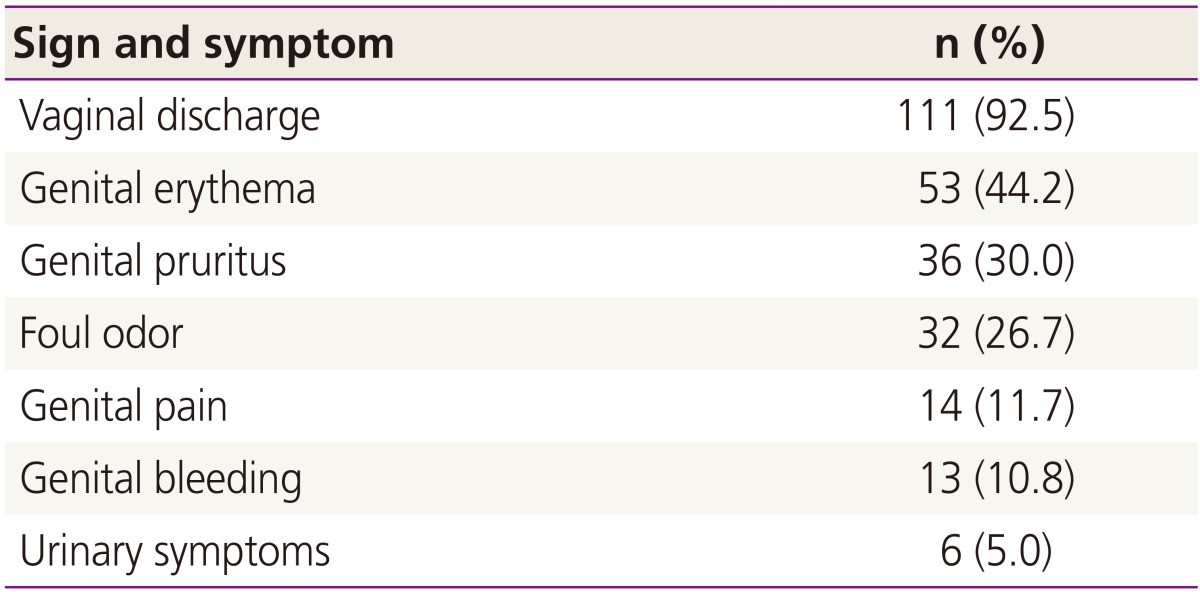
The frequency of signs and symptoms are shown in Table 1. Vaginal discharge was the most frequent symptom in this patient group; it was reported for 92% of patients as a subjective symptom or an objective finding. Genital erythema and pruritus were reported in 44% and 30% of subjects, respectively. Genital bleeding or a bloody discharge was reported in 11% of subjects. As a matter of course, a thorough history had been taken and careful genital examination had been performed for these patients to exclude other causes of pediatric vaginal bleeding.
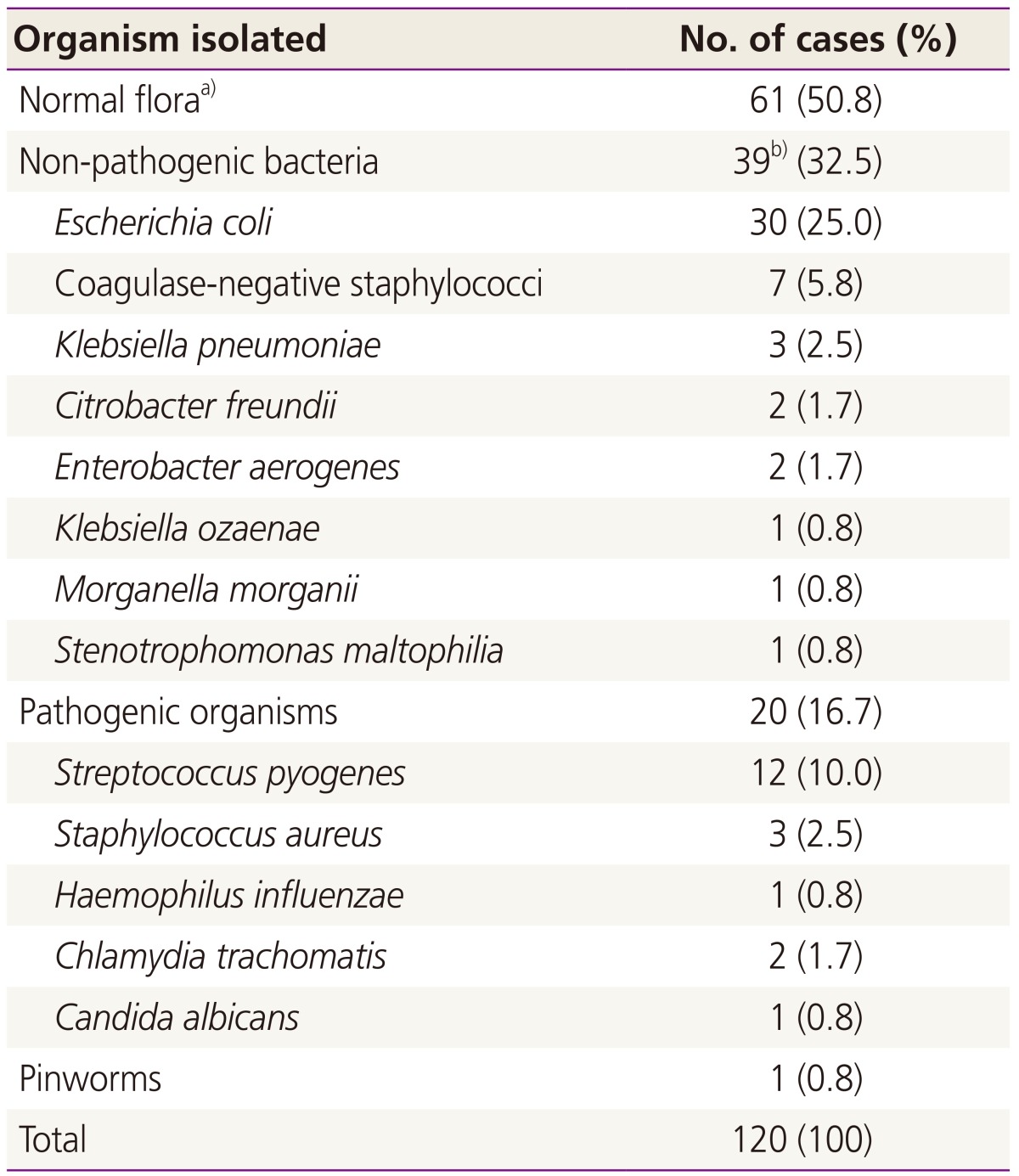
Microbiologic investigation revealed normal flora (n=61, 50.8%) or non-pathogenic bacteria (n=39, 32.5%) in the majority of patients (n=100, 83.3%) (Table 2). Escherichia coli were the most commonly identified non-pathogenic bacteria (n=30, 25%).
Pathogenic organisms were isolated in 16.7% of the patients (n=20). The respiratory pathogens Streptococcus pyogenes (n=12, 10.0%), Staphylococcus aureus (n=3, 2.5%), and Haemophilus influenzae (n=1, 0.8%) were specifically identified. Candida albicans was detected in 1 patient (0.8%), a 2-year-old girl who was not yet toilet trained. Chlamydial antigen polymerase chain reaction tests were selectively performed in 7 children with abnormal hymenal configuration; a positive result was identified in 2 children (1.7%). Pinworm was reported in a 5-year-old girl with symptoms of genital itching and vaginal discharge. There were no cases of Shigella or Yersinia reported, even in one patient with accompanying diarrhea.
Fig. 3 illustrates the seasonal distribution of genital microorganisms in 116 patients. The 4 cases that had presented with Chlamydia trachomatis, Candida albicans, and pinworm were excluded. There were no obvious seasonal traits found in any microorganism subgroup; however, the vulvovaginitis cases that were associated with respiratory pathogens seemed to occur more frequently in summer and winter.
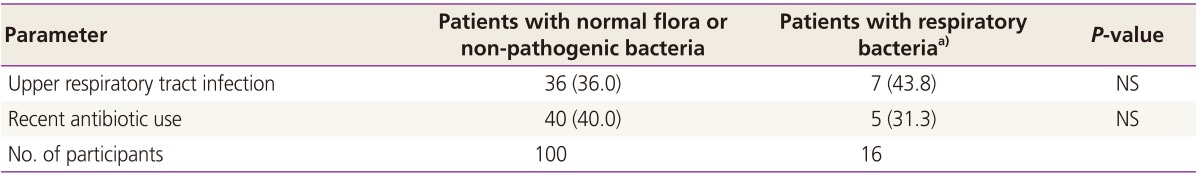
A history of URI in the previous month was reported in 45 (37.5%) patients with vulvovaginitis (data not shown). In addition, recent swimming or bubble bath use was reported by 15.8% (n=19) and 10.0% (n=12), respectively. A significant proportion of the patients had a recent history of antibiotic use (n=48, 40%). A history of antibiotic use was more common in patients with normal flora or non-pathogenic bacteria compared to patients with respiratory pathogens; however, the difference was not statistically significant (P>0.05) (Table 3). Furthermore, a recent history of URI was slightly more common in patients with respiratory pathogens, but this difference also failed to achieve statistical significance (P>0.05).
Children who had presented with severe clinical symptoms requiring prompt management with antibiotics, those who had received antibiotic treatment for non-gynecologic causes in the indicated period, or those who had been found to have specific pathogens, such as Chlamydia trachomatis, Candida albicans, and pinworms, were excluded from this analysis (n=16).
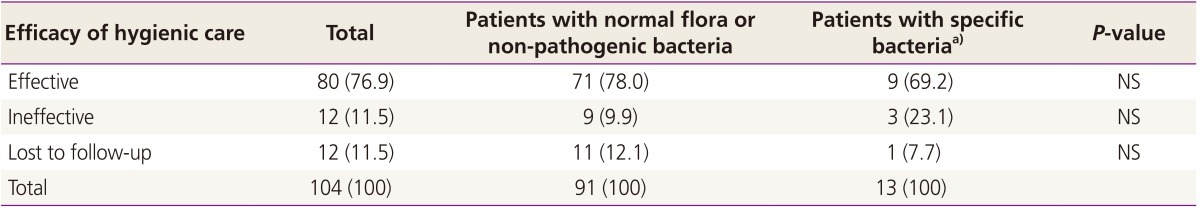
Of 104 patients who were assessed for the efficacy of perineal hygienic care, 80 (76.9%) achieved a partial or complete improvement of genital symptoms without the need for oral antibiotics (Table 4). Treatment failure was reported in 12 patients (11.5%) for whom a prescription for oral antibiotics was provided on their second visit. Twelve (11.5%) children did not attend their second appointment; therefore, efficacy in these cases could not be established. The efficacy of hygienic care was not significantly different between patients with or without specific pathogens (P>0.05).
The diagnosis of pediatric vulvovaginitis is complicated by uncertainty in the categorization of normal microflora and potential pathogens. The normal vaginal flora of prepubertal girls is not well established, but several studies have reported predominant microflora in the lower genital tract of healthy children [9,10,11,12]. Non-specific vulvovaginitis typically presents with normal flora or non-pathogenic bacteria, and is commonly triggered by poor hygienic conditions or genital irritants [12]. In our study, normal flora or non-pathogenic organisms were isolated in 83.3% (n=100) of patients, compatible with the non-specific vulvovaginitis cases. Previous studies have reported lower rates of non-specific vulvovaginitis, between 25% and 75% (12). Despite a high rate of non-specific infection, the rate of Escherichia coli (25%, n=30) was relatively low in our study compared to other studies in children with vaginitis [10,11]. Although we did not have a control group, the frequency of Escherichia coli in our study was similar to that reported for asymptomatic children in another study [10].
The rate and entity of specific microorganisms associated with pediatric vulvovaginitis have been studied since the 1950s. Early studies reported varying rates, ranging from 10% to 50%, as well as dissimilar entities of specific pathogens [1,2,13]. Interestingly, earlier studies reported relatively high rates of gonorrhea [1,13,14] or pinworm infestation [2], which might reflect the socioeconomic conditions at that time. Meanwhile, studies conducted in the past 20 years have reported more consistent rates, ranging from 20% to 40%, of cases involving specific pathogens, mainly respiratory bacteria such as Streptococcus pyogenes, Haemophilus influenzae, or Staphylococcus aureus [5,7,8]. In our study, specific pathogens were found in 16.7% (n=20) of subjects, and respiratory pathogens accounted for 80.0% of the specific vulvovaginitis cases. The rate of specific infection in this study is similar to that reported in a previous Korean study published in 1999 [6], but relatively low compared to other studies [5,7]. The exact cause of the low frequency of specific pathogens in our study is not known; however, the substantial proportion of patients with a history of recent antibiotic use (40%) in our study is likely to have affected the results of bacterial culture.
The frequency of detection of Streptococcus pyogenes, Staphylococcus aureus, and Haemophilus influenzae in our patients with specific vulvovaginitis was 60%, 15%, and 5%, respectively. Compared to a previous Korean study, the prevalence of Haemophilus influenzae is substantially lower, whereas that of Streptococcus pyogenes is higher [6]. This difference over time has also been reported elsewhere. In a study from 1992, Haemophilus influenzae was reported as the most frequent specific bacteria in 200 girls presenting with genital discharge [2]. However, since 2000, Streptococcus pyogenes has become the most commonly identified specific pathogen in the majority of studies investigating pediatric vulvovaginitis [3,7,8,15]. It is possible that the Haemophilus influenzae vaccination, widely adopted since the 1980s, has reduced the incidence of vulvovaginitis caused by this organism [7]. The increase in frequency of cases involving Streptococcus pyogenes is probably related to the increase in cases of streptococcal pharyngitis [3,16].
We also analyzed the seasonal distribution of presentation to hospital and the time of symptom onset. Hospital visits increased significantly in the summer and winter, but this trend was attenuated in the analysis of time of symptom onset (Fig. 2). The greater convenience of hospital visits during vacation periods may potentially affect the seasonal distribution of presentation to hospital. The frequency of cases associated with respiratory pathogens increased slightly in the summer and winter, but the trend was not distinct (Fig. 3). One study reported the peak incidence of perineal streptococcal infection in winter and spring [17], but another study failed to demonstrate any distinct seasonal traits in cases of vulvovaginitis caused by Streptococcus pyogenes [7].
Many studies have provided support for the hypothesis of transmission of an URI to the perineal area by autoinoculation or gastrointestinal spread [7,16,17,18]. The rate of concurrence between URI and perineal culture results is variable, but has been reported up to 92% [17]. The variability observed is probably related to the interval between the expression of the URI and the time of diagnosis because respiratory pathogens may be eliminated from the upper respiratory tract with time. In our study, the frequency of URI was not significantly different between patients with or without respiratory pathogens (P>0.05). However, this finding does not refute the correlation between URI and vulvovaginitis because of the lack of pharyngeal culture tests in our study, and the varying intervals between the onset of symptoms and diagnosis.
Typically, patients with non-specific vulvovaginitis are primarily treated with hygienic measures, and oral antibiotics are provided if specific bacteria, especially Streptococcus pyogenes, are detected [2,4,19,20]. However, in our study, the efficacy of hygienic care was similar in patients with or without specific pathogens (P>0.05). Almost 70% of patients with specific pathogens were successfully treated with hygienic care and did not require oral antibiotics. To our knowledge, this is the first study to report the successful use of perineal hygienic care as treatment for patients with specific vulvovaginitis.
The strength of this study lies in the use of recent, relatively large-scale samples of pediatric vulvovaginitis. There are 2 major limitations in our study design. First, the lack of a control group, and second, the use of a retrospective medical record review, which limited our ability to collect a uniformed patient dataset and to analyze the treatment outcomes. While the Chi-square test evaluated the efficacy of hygienic care, a significant proportion (11.5%) of missing data may have affected the statistical power of the analysis.
In conclusion, this study has demonstrated relatively low rates of pediatric vulvovaginitis associated with specific pathogens in Korea. Streptococcus pyogenes was the leading cause of specific vulvovaginitis, and no cases involved enteric pathogens, such as Shigella or Yersinia. In addition, our study demonstrated the successful use of perineal hygienic care in patients with specific vulvovaginitis.
References
1. Paradise JE, Campos JM, Friedman HM, Frishmuth G. Vulvovaginitis in premenarcheal girls: clinical features and diagnostic evaluation. Pediatrics 1982;70:193-198. PMID: 7099784.


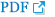
2. Pierce AM, Hart CA. Vulvovaginitis: causes and management. Arch Dis Child 1992;67:509-512. PMID: 1580682.



3. Cuadros J, Mazon A, Martinez R, Gonzalez P, Gil-Setas A, Flores U, et al. The aetiology of paediatric inflammatory vulvovaginitis. Eur J Pediatr 2004;163:105-107. PMID: 14655013.


4. Joishy M, Ashtekar CS, Jain A, Gonsalves R. Do we need to treat vulvovaginitis in prepubertal girls? BMJ 2005;330:186-188. PMID: 15661783.



5. Cox RA. Haemophilus influenzae: an underrated cause of vulvovaginitis in young girls. J Clin Pathol 1997;50:765-768. PMID: 9389978.



6. Kim HC, Lee MH, Hong SG. Pediatric vulvovaginitis: a study of clinical and microbiologic features and the efficacy of perineal hygienic care. Korean J Obstet Gynecol 1999;42:2821-2828.
7. Stricker T, Navratil F, Sennhauser FH. Vulvovaginitis in prepubertal girls. Arch Dis Child 2003;88:324-326. PMID: 12651758.



8. Yilmaz AE, Celik N, Soylu G, Donmez A, Yuksel C. Comparison of clinical and microbiological features of vulvovaginitis in prepubertal and pubertal girls. J Formos Med Assoc 2012;111:392-396. PMID: 22817817.


9. Hammerschlag MR, Alpert S, Rosner I, Thurston P, Semine D, McComb D, et al. Microbiology of the vagina in children: normal and potentially pathogenic organisms. Pediatrics 1978;62:57-62. PMID: 98750.


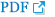
10. Gerstner GJ, Grunberger W, Boschitsch E, Rotter M. Vaginal organisms in prepubertal children with and without vulvovaginitis: a vaginoscopic study. Arch Gynecol 1982;231:247-252. PMID: 6751240.


11. Jaquiery A, Stylianopoulos A, Hogg G, Grover S. Vulvovaginitis: clinical features, aetiology, and microbiology of the genital tract. Arch Dis Child 1999;81:64-67. PMID: 10373139.



12. Emans SJ. Vulvovaginal problems in the prepubertal child. In: Emans SJ, Laufer MR, editors. Pediatric and adolescent gynecology. 6th ed. Philadelphia (PA): Lippincott Williams & Wilkins; 2012. p. 42-59.
14. Shapiro RA, Schubert CJ, Siegel RM. Neisseria gonorrhea infections in girls younger than 12 years of age evaluated for vaginitis. Pediatrics 1999;104:e72PMID: 10586006.


15. McGreal S, Wood P. Recurrent vaginal discharge in children. J Pediatr Adolesc Gynecol 2013;26:205-208. PMID: 22264471.


16. Hansen MT, Sanchez VT, Eyster K, Hansen KA. Streptococcus pyogenes pharyngeal colonization resulting in recurrent, prepubertal vulvovaginitis. J Pediatr Adolesc Gynecol 2007;20:315-317. PMID: 17868900.


17. Mogielnicki NP, Schwartzman JD, Elliott JA. Perineal group A streptococcal disease in a pediatric practice. Pediatrics 2000;106(2 Pt 1):276-281. PMID: 10920151.


18. Straumanis JP, Bocchini JA Jr. Group A beta-hemolytic streptococcal vulvovaginitis in prepubertal girls: a case report and review of the past twenty years. Pediatr Infect Dis J 1990;9:845-848. PMID: 2263434.


19. Sharma B, Preston J, Greenwood P. Management of vulvovaginitis and vaginal discharge in prepubertal girls. Rev Gynaecol Pract 2004;4:111-120.

20. Dei M, Di Maggio F, Di Paolo G, Bruni V. Vulvovaginitis in childhood. Best Pract Res Clin Obstet Gynaecol 2010;24:129-137. PMID: 19884044.


Fig. 2
Seasonal distribution of (A) presentation to clinic, and (B) time of symptom onset in prepubertal girls with vulvovaginitis (n=120).
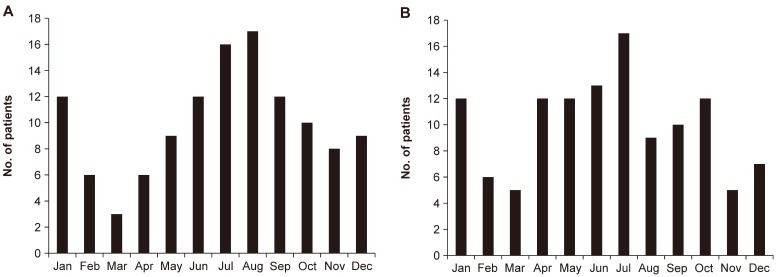
Fig. 3
Seasonal distribution of genital microorganisms in prepubertal girls with vulvovaginitis (n=116a)). a)Of the 120 study participants, 4 patients who presented with Chlamydia trachomatis (n=2), Candida albicans (n=1), and pinworms (n=1) were excluded.
Table 2
Organisms isolated from the genital specimens of prepubertal girls with vulvovaginitis (n=120)
-
METRICS

-
- 11 Crossref
- 3,191 View
- 41 Download
- Related articles in Obstet Gynecol Sci