 |
 |
- Search
| Obstet Gynecol Sci > Volume 60(1); 2017 > Article |
Abstract
Lymphoepithelioma-like carcinoma (LELC) of the uterine cervix is exceedingly uncommon. We herein report a rare case of cervical LELC. A 45-year-old woman was admitted to gynecology department with vaginal bleeding for one month. Liquid-based cytology revealed atypical endometrial cells, not otherwise specified on her cervix. On a hysteroscopy, an endocervical mass was identified and the pathologic result was consistent with poorly differentiated squamous cell carcinoma. Magnetic resonance imaging and positron emission tomography with 2-deoxy-2-[fluorine-18] fluoro-D-glucose integrated with computed tomography revealed a 3.1-cm endocervical mass without distant metastasis or enlarged lymph nodes. The International Federation of Gynecology and Obstetrics stage was IB1. A radical hysterectomy and bilateral pelvic lymph node dissection were performed. The pathologic diagnosis was a poorly differentiated carcinoma, showing features of LELC. She has been followed for 8 months without adjuvant treatment since the surgery, during which time there has been no evidence of tumor recurrence or metastasis.
Lymphoepithelioma carcinoma is a common type of poorly-differentiated epithelial cells in the nasopharynx [1,2,3]. Histologically, it appears as nests of poorly-differentiated malignant cells with syncytial growth patterns. It is associated with noticeable lymphocytic stromal infiltration. Studies on lymphoepithelioma carcinoma in the nasopharynx have found that the condition is more prevalent in Asian populations, and that it is related to Epstein-Barr virus (EBV) infection and favorable clinical outcomes [1,4]. Neoplasia with characteristics that are similar to those of nasopharyngeal lymphoepithelioma carcinoma occurring at anatomic sites other than the nasopharynx, such as the salivary glands, lungs, thymus, stomach, and uterine cervix, are referred to as lymphoepithelioma-like carcinoma (LELC) [3]. LELC of the uterine cervix is very rare; it accounts for only 0.63% of all cases of primary uterine cervical carcinoma in the Western world and about 5.5% of those in Japan [1,5]. A literature search about cervical LELC in PubMed uncovered only 3 English language original articles [1,3,5] and 9 English language case reports on 16 patients [2,4,6,7,8,9,10,11,12]. So far, only 3 case reports in Korean journals of obstetrics and gynecology have been published [13,14,15]. In the World Health Organization histological classification of tumors of the uterine cervix, LELC is classified as a subtype of squamous cell carcinoma [4]. Though LELC is histologically poorly differentiated, its clinical prognosis is better than that of other squamous cell carcinomas of the uterine cervix. For this reason, being able to identify the differences between LELC and other poorly-differentiated squamous cell carcinomas, lymphomas, and other lymphoproliferative disorders of the cervix is very important for correct diagnosis and treatment [2]. Some studies have found that EBV is associated with the pathogenesis of cervical LELC, especially in Asian woman [3]. However, this issue remains controversial. We herein present a case of LELC of the cervix in a 45-year-old Korean woman along with a literature review.
A 45-year-old, premenopausal, Korean woman, gravida 4, parity 2, was referred to the department of obstetrics and gynecology of Pusan National University Yangsan Hospital. She visited another hospital because of vaginal bleeding that had persisted for one month. A cervical liquid-based cytology test was performed, which revealed atypical endometrial cells not otherwise specified. Endometrial sampling was recommended. On hysteroscopy, an endocervical mass was identified. A biopsy taken from the endocervical mass revealed poorly differentiated squamous cell carcinoma. The patient visited our hospital for further assessment and treatment of cervical cancer. The results of a colposcopy were unsatisfactory due to no visible transformation zone. On bimanual examination, the parametrium was soft without a palpable mass. Her past medical history was unremarkable. Her hematological profile revealed a hemoglobin level of 8.4 g/dL with normal leukocyte and platelet counts. The serum level of squamous cell carcinoma antigen (0.9 ng/mL) was within normal limits. A human papilloma virus (HPV) DNA chip test following cytobrushing of the cervix did not detect high risk HPV DNA. Magnetic resonance imaging (Fig. 1A) and positron emission tomography with 2-deoxy-2-[fluorine-18] fluoro-D-glucose integrated with computed tomography revealed a 3.1-cm mass at the anterior aspect of the endocervix and multiple uterine myomas, all of which were less than 9 cm. No distant metastatic lesions or enlarged lymph nodes were observed. The patient was clinically diagnosed as International Federation of Gynecology and Obstetrics (FIGO) stage IB1, with no infiltration of the vaginal wall or parametrium. A radical hysterectomy and bilateral pelvic lymph node dissection, and transposition of both ovaries were performed to treat cervical cancer. Grossly, pathologic lesion was invisible in exocervix. The uterine cervix was opened at 12 o'clock (Fig. 1B). On gross section, the endocervix contained a relatively well-defined brownish-white depressed mass at 12 to 6 o'clock, which measured 2.4├Ś0.9 cm in size. It was 4.2 cm away from the closest vaginal cuff margin. It invaded to a depth of about 0.9 cm in the 1.5-cm-thick cervical wall. Given the macroscopic findings, the relatively well-defined endocervical mass appeared.
On microscopic examination, poorly-differentiated epithelioid cells were evident, which were made up of clusters surrounded by markedly infiltrated lymphoid cells. Because this is the typical pattern of LELC, the condition could be recognized easily even at low magnification. The cancer cells showed large, ill-defined cytoplasmic borders, abundant cytoplasm, prominent nucleoli, and syncytial growth patterns (Fig. 1C). Lymphovascular invasion, perineural invasion, and lymph node metastasis were not present. in situ hybridization for EBV-encoded early RNAs was done in formalin-fixed paraffin-embedded tissue. The result was negative (Fig. 1D). And the result of HPV polymerase chain reaction in paraffin-embedded tissue was negative. The postoperative course was uneventful, and the patient left the hospital 7 days after surgery. The final pathologic results revealed LELC of cervix. The patient has been followed up for eight months without adjuvant treatment, with an abdominal computed tomography scan taken after 6 months from surgery in an outpatient clinic, which revealed no evidence of recurrence or metastasis.
LELC of the uterine cervix is a rare variant of poorly-differentiated squamous cell carcinoma. The review of previously published cases and original articles of LELC are listed in Table 1 [1,2,3,4,5,6,7,8,9,10,11,12,13,14,15]. It is made up of sheets showing a syncytial growth pattern with marked infiltration of lymphocytes in the stroma [2,3,5]. The incidence of cervical LELC in Asians is higher than in the Western population, just as the incidence of nasopharyngeal lymphoepithelioma carcinoma is higher in the Asian than in the Western population.
Generally, cervical LELC occurs at a younger age than do other types of cervical carcinoma. In 1977, Hasumi et al. [5] reported that 16 of 39 cervical LELC patients with a mean age of 43.5 years were less than 40 years old. In cases of other cervical carcinomas, only 28.2% (mean age, 48.6 years) of patients were less than 40 years old. Our patient was 45 years old, premenopausal woman, which is close to the mean age of cervical LELC patients but she was younger than LELC patients who were reported in Korean cases.
Although the morphological features of cervical LELC appear aggressive, the prognosis is better than that for other type of squamous cell carcinomas of the uterine cervix. In comparison with other carcinomas of the same FIGO stage, cervical LELC is characterized by less regional lymph node metastasis [5]. Tseng et al. [3] reported that, even in other organs, LELC tumors are associated with good clinical outcomes. The hypothesis for the good prognosis is that tumors may induce both humoral and cell-mediated immunologic reactions [5]. Some reports have suggested that the good prognosis may be related to the immunologic reaction caused by tumor-associated antigens, which are the host's response to lymphocytic infiltration. The infiltrated lymphocytes found in the stroma reflect the humoral and cell-mediated immune response to tumors. The response seems to reduce lymph node metastasis and increase the overall survival rate [1,5]. In our case, there were no lymphovascular, perineural, parametrial, or vaginal invasions, and no lymph node metastasis. The patient exhibited characteristics typical of cervical LELC.
Saroha et al. [4] reported that when a cervical LELC specimen is obtained from a highly inflammatory lesion or obscure tumor cells, an exact diagnosis is very difficult. For differential diagnosis of vague biopsy lesions, immunohistochemical staining for cytokeratin or epithelial membrane antigen is necessary. Tseng et al. [3] reported that 4 of 15 cervical LELC patients showed poorly-differentiated carcinoma on cervical biopsies taken by colposcopy, whereas the other 11 patients with cervical LELC were diagnosed histologically after radical hysterectomy. A diagnosis of cervical LELC with only a biopsy specimen is difficult. Therefore, an assessment of a hysterectomy specimen is needed for accurate diagnosis. Moreover, LELC of the uterine cervix is an important differential diagnosis, and should not be confused with other types of poorly-differentiated squamous cell carcinomas and prominent lymphoid-related neoplasia in the stroma, such as glassy cell carcinoma, which have poor prognoses [4,5]. In our case, an initial cervical biopsy from endocervical mass showed poorly-differentiated squamous cell carcinoma. The diagnosis was confirmed after radical hysterectomy. The difference between our case and other LELC cases is that our case showed endocervical mass which is found by hysteroscopy. We had a chance for pathologic diagnosis before the operation.
EBV is thought to be an oncogenic factor in lymphoepithelioma carcinoma of the nasopharynx. This knowledge is more relevant to Asian patients than to those of other ethnicities [3]. However, the clinical pathogenesis of LELC in the cervix remains controversial. Some reports suggest that EBV is an etiologic factor in LELC of the uterine cervix. One report on Taiwanese women with cervical LELC found that EBV was present, as identified by polymerase chain reaction for EBV DNA, in 73.3% (11/15) of 15 LELC patients [3]. However, Chao et al. [1] reported that, of 9 Taiwanese women with uterine cervical LELC, none had EBV, as assayed by in situ hybridization for EBV-encoded early RNAs. It has been suggested that EBV does not act as a carcinogenic factor in cervical LELC, but the EBV DNA sequence may be found in lymphocytes that have infiltrated the stroma. In Western women, EBV has never been confirmed to be a factor in cervical LELC [6,7,8,9]. These findings imply that race and geographic factors may influence the role of the EBV gene as an oncogenic factor in uterine cervical LELC [3].
Some reports have demonstrated the influence of HPV as causative agent in cervical LELC in Western women. However, pathogenesis related to the interaction between the virus and epithelioid cells is unclear and controversial [6,8,10]. The prognosis of cervical LELC is favorable. After surgery, the result of therapeutic response is good.
In conclusion, LELC is rare and difficult to diagnose. Therefore, large-scale research is difficult to conduct. A multicenter, national registration system could be essential for future research about the prognosis and treatment of such a rare disease.
References
1. Chao A, Tsai CN, Hsueh S, Lee LY, Chen TC, Huang SL, et al. Does Epstein-Barr virus play a role in lymphoepithelioma-like carcinoma of the uterine cervix? Int J Gynecol Pathol 2009;28:279-285. PMID: 19620947.


2. Takai N, Nakamura S, Goto K, Hayashita C, Kira N, Urabe S, et al. Lymphoepithelioma-like carcinoma of the uterine cervix. Arch Gynecol Obstet 2009;280:725-727. PMID: 19238413.


3. Tseng CJ, Pao CC, Tseng LH, Chang CT, Lai CH, Soong YK, et al. Lymphoepithelioma-like carcinoma of the uterine cervix: association with Epstein-Barr virus and human papillomavirus. Cancer 1997;80:91-97. PMID: 9210713.


4. Saroha V, Gupta P, Singh M, Dhingra K, Khurana N. Lymphoepithelioma-like carcinoma of the cervix. J Obstet Gynaecol 2010;30:659-661. PMID: 20925604.


5. Hasumi K, Sugano H, Sakamoto G, Masubuchi K, Kubo H. Circumscribed carcinoma of the uterine cervix, with marked lymphocytic infiltration. Cancer 1977;39:2503-2507. PMID: 872050.


6. Bais AG, Kooi S, Teune TM, Ewing PC, Ansink AC. Lymphoepithelioma-like carcinoma of the uterine cervix: absence of Epstein-Barr virus, but presence of a multiple human papillomavirus infection. Gynecol Oncol 2005;97:716-718. PMID: 15863191.


7. Martorell MA, Julian JM, Calabuig C, Garcia-Garcia JA, Perez-Valles A. Lymphoepithelioma-like carcinoma of the uterine cervix. Arch Pathol Lab Med 2002;126:1501-1505. PMID: 12456211.


8. Noel J, Lespagnard L, Fayt I, Verhest A, Dargent J. Evidence of human papilloma virus infection but lack of Epstein-Barr virus in lymphoepithelioma-like carcinoma of uterine cervix: report of two cases and review of the literature. Hum Pathol 2001;32:135-138. PMID: 11172309.


9. Lopez-Rios F, Miguel PS, Bellas C, Ballestin C, Hernandez L. Lymphoepithelioma-like carcinoma of the uterine cervix: a case report studied by in situ hybridization and polymerase chain reaction for Epstein-Barr virus. Arch Pathol Lab Med 2000;124:746-747. PMID: 10782160.


10. Saylam K, Anaf V, Fayt I, Noel JC. Lymphoepithelioma-like carcinoma of the cervix with prominent eosinophilic infiltrate: an HPV-18 associated case. Acta Obstet Gynecol Scand 2002;81:564-566. PMID: 12047313.


11. Takebayashi K, Nishida M, Matsumoto H, Nasu K, Narahara H. A case of lymphoepithelioma-like carcinoma in the uterine cervix. Rare Tumors 2015;7:5688PMID: 25918614.



12. Kaul R, Gupta N, Sharma J, Gupta S. Lymphoepithelioma-like carcinoma of the uterine cervix. J Cancer Res Ther 2009;5:300-301. PMID: 20160367.


13. Kim ML, You HJ, Yoon ES, Sim SH, Koo BS, Joo WD, et al. A case of lymphoepithelioma-like carcinoma of the uterine cervix. Korean J Obstet Gynecol 2007;50:207-211.
14. Ki EY, Ro DY, Kim HJ, Park BJ, Kim YW, Kim TE, et al. A case of lymphoepithelioma-like carcinoma of the uterine cervix. Korean J Obstet Gynecol 2009;52:115-119.
15. Yoo YS, Hur JY, Yang MH. A case of lymphoepitheliomalike carcinoma of the uterine cervix. Korean J Obstet Gynecol 2001;44:176-179.
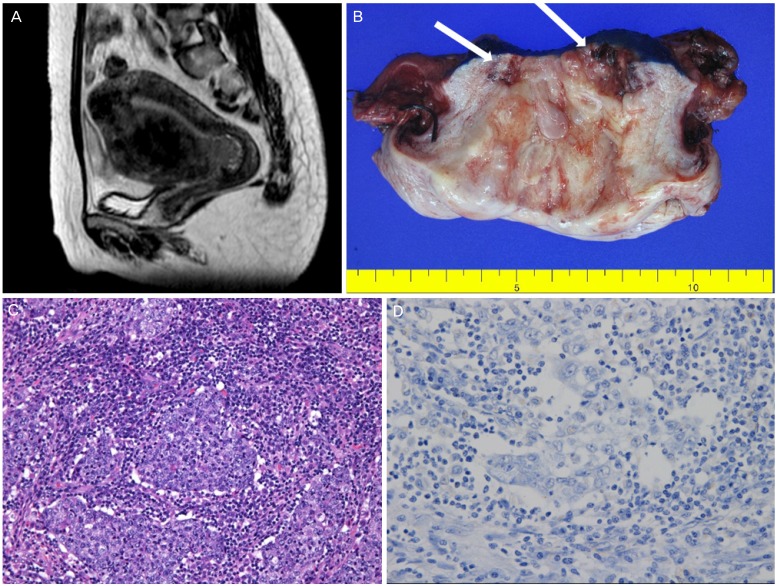
Fig.┬Ā1
(A) Sagittal T2-weighted magnetic resonance imaging scan revealing a well-defined high signal intensity mass, 3.1 cm in size, at the anterior aspect of the endocervix, along with multiple uterine myomas less than 9 cm in size. (B) Macroscopically, the cervix was open at 12 o'clock. (C) The cells had large, ill-defined cytoplasmic borders, abundant cytoplasm, prominent nucleoli, and syncytial growth patterns (H&E, ├Ś200). (D) Formalin fixed paraffin-embedded tissue used for in situ hybridization for Epstein-Barr virus-encoded early RNAs. The result was negative.
Table┬Ā1
Literature review of lymphoepithelioma-like carcinoma of cervix
EBV, Epstein-Barr virus; HPV, human papilloma virus; FIGO, International Federation of Gynecology and Obstetrics; RH, radical hysterectomy; BPLND, bilateral pelvic lymph node dissection; PALND, para-aortic lymph node dissection; BSO, bilateral salpingo-oophorectomy; TAH, total abdominal hysterectomy.
| Author | Country | Article type | No. of case | Age (yr) (or median) | EBV | HPV | FIGO stage | Treatment | Adjuvant treatment | Follow-up (mo) (median) | Follow-up status |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Chao et al. [1] | Taiwan | Original article | 9 | 54 (40-67) | Negative | 16(3), 18,31,35, 58, 16/58 | IB | RH, BPLND | Radiotherapy | Mean 112 ( 63-134 ) | No recur |
| Tseng et al. [3] | Taiwan | Original article | 15 | 56 (37-72) | Positive (73%, 11/15) | 16 (20%, 3/15) | IB (9/15) | RH, BPLND (10/15) | Mean 45 ( 20-63 ) | No recur | |
| IIA (2/15) | Radiotherapy (5/15) | ||||||||||
| IIB (4/15) | |||||||||||
| Hasumi et al. [5] | Japan | Original article | 39 | 43.5 (30-61) | Not done | Not done | IB | RH | Mean 58.5 ( 3-60 ) | No recur | |
| Takai et al. [2] | Japan | Case | 3 | 41 | Negative | Negative | IB1 | RH, BPLND | No report | 100 | No recur |
| 69 | Negative | Negative | IIA | RH, BPLND | No report | 75 | No recur | ||||
| 44 | Negative | Negative | IB1 | RH, BPLND | No report | 15 | No recur | ||||
| Saroha et al. [4] | India | Case | 2 | 40 | Not done | Not done | IB1 | RH, BPLND, PALND | No report | 14 | No recur |
| 43 | Not done | Not done | IB1 | RH, BSO, BPLND, PALND | No report | 12 | No recur | ||||
| Bais et al. [6] | Netherlands | Case | 1 | 44 | Negative | 16, 45 | IB1 | RH, BPLND | None | No report | No recur |
| Martorell et al. [7] | Spain | Case | 4 | 74 | Negative | Negative | IB1 | Cervicectomy | No report | 84 | No recur |
| 58 | Negative | Negative | IB1 | RH, BPLND | No report | 60 | No recur | ||||
| 77 | Negative | Negative | II | RH, BPLND | No report | 24 | No recur | ||||
| 67 | Negative | Negative | IB1 | RH, BPLND | No report | 24 | Recur | ||||
| Noel et al. [8] | Belgium | Case | 2 | 56 | Negative | 16 | IB1 | RH, BPLND | No report | No report | No recur |
| 53 | Negative | 18 | IB1 | RH, BPLND | No report | 24 | No recur | ||||
| Lopez-Rios et al. [9] | Spain | Case | 1 | 44 | Positive | Not done | IB1 | RH, BPLND | No report | 12 | No recur |
| Saylam et al. [10] | Belgium | Case | 1 | 72 | Not done | 18 | IB1 | RH, BPLND | None | No report | No recur |
| Takebayashi et al. [11] | Japan | Case | 1 | 45 | Negative | Not done | IB2 | RH | Radiotherapy | 4 | No recur |
| Kaul et al. [12] | India | Case | 1 | 42 | Not done | Not done | IB1 | RH, BPLND | No report | 12 | No recur |
| Kim et al. [13] | Korean | Case | 1 | 57 | Negative | Negative | IB1 | RH, BSO, BPLND, PALND, appendectomy | Paclitaxel + cisplatin | 26 | No recur |
| Ki et al. [14] | Korean | Case | 1 | 63 | Positive | 16 | IB1 | RH, BSO, BPLND, appendectomy | None | 34 | No recur |
| Yoo et al. [15] | Korean | Case | 1 | 55 | Not done | Not done | IB1 | RH, BSO, BPLND | None | 12 | No recur |
-
METRICS

- Related articles in Obstet Gynecol Sci
-
Flow cytometric analysis of DNA patterns in carcinoma of the uterine cervix.1991 September;34(9)
Adenocarcinoma of the uterine cervix: clinical and histologic variables.1991 October;34(10)
A case of glassy cell carcinoma of the uterine cervix.1992 March;35(3)




















