|
 |
- Search
| Obstet Gynecol Sci > Volume 56(2); 2013 > Article |
Abstract
We describe a case in which homonymous hemianopsia developed abruptly following an epidural blood patch procedure. The procedure was performed in a patient complaining of post-dural puncture headache after an emergency Cesarean section under spinal anesthesia. Computed tomography and magnetic resonance imaging demonstrated that air bubbles had moved from the prepontine and premedullar cisterns toward the left retrochiasmal region. The homonymous hemianopsia resolved rapidly with conservative management including oxygen, intravenous fluid, and antibiotics. We report on this case with a brief review of the related literature.
Homonymous hemianopsia is a specific visual disturbance induced by the lesions of the retrochiasmal visual pathways, including the optic tract, lateral geniculate body, parietotemporal radiation, and occipital cortex [1]. The most frequent cause is apoplexy, followed by trauma, neoplasm, brain surgery, and other less common mechanisms [1-3]. We report on an occurrence of temporary homonymous hemianopsia after spinal anesthesia and epidural blood patch. One common side effect of spinal anesthesia, which is often performed during operations in the lower abdomen and pelvis, is a headache due to a cerebrospinal fluid leak from a dural puncture. An epidural blood patch (EBP) procedure using autologous blood is commonly performed for post-dural puncture headache (PDPH). Pneumocephalus may occur because of the presence of within the dural space during spinal puncture or EBP procedures, and subsequent nerve-related symptoms may appear.
The authors report on a unique case of temporary homonymous hemaniopsia after EBP due to pneumocephalus and briefly review the literature.
A 33-year-old pregnant woman had been transferred to our outpatient clinic with the concern for preterm labor at 23 weeks gestation but was ultimately sent home. After a triplet pregnancy achieved through an in vitro fertilization embryo transfer in a private clinic, the patient underwent a McDonald operation at 16 weeks gestation due to the risk of preterm birth in multiple gestations. The patient then presented to the emergency department of our hospital at 30 weeks and 2 days gestation due to premature rupture of membranes. She was prepared for an urgent Caesarean section at 31 weeks and 3 days gestation due to sudden contractions. In a seated position, the patient underwent a midline approach to the L3-4 interspinous space using an 18 G Tuohy needle. Cerebrospinal fluid leaked while identifying the epidural space using the loss of resistance (LOR) technique with 2.5 mL of air. Dural puncture was suspected, and the needle was removed. As a result, the initially scheduled epidural anesthesia was changed to spinal anesthesia. Subsequently, we successfully initiated spinal anesthesia using a 26 G Quincke needle in the same location. The patient was move to a supine position after administering 10 mg of bupivacaine. The Caesarean section was initiated after confirmation of adequate anesthesia up to the fourth thoracic segment. All three babies and the placenta were delivered. All vital signs were stable before and after the anesthetic injection, and no abnormal findings were observed at the time of the procedure. The patient was advised postoperative bed rest and began early ambulation on the first postoperative day. Since the patient complained of mild tinnitus during ambulation without any other associated symptoms, closer follow-up was initiated.
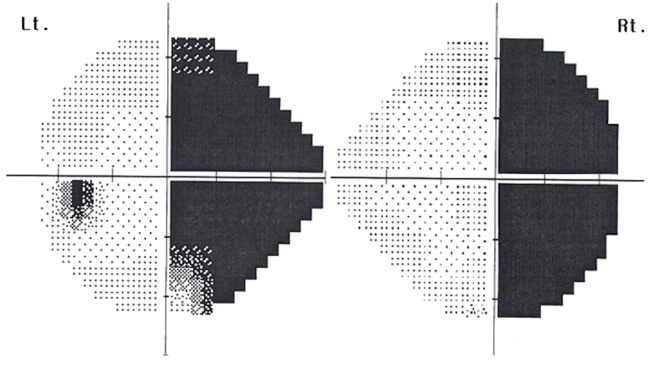
On the second postoperative day, she complained of headache, nausea, and other symptoms, and she began complaining of a stiff neck and vomiting on the third postoperative day. These symptoms were alleviated in the supine position but recurred when the patient assumed standing or sitting positions. No other focal neurologic symptoms were identified at that time, and vital signs were stable. Despite conservative management including bed rest, the administration of fluid, analgesics and anti-nauseants, her symptoms persisted. The patient was sent to the Department of Neurology on the fourth postoperative day for suspected PDPH. She was encouraged to undergo epidural blood patch. We were initially planning to perform EBP after the confirmation of PDPH based on computed tomography (CT) scans; however, the scanning was delayed after the procedure due to limited availability. Subsequently, the patient was placed in the left lateral position, and the epidural space was identified using about 2.5 mL of air with the LOR technique at the L4-5 spinal level. No leakage of cerebrospinal fluid was detected at that time. Fifteen milliliters of the patient's own blood were injected using an aseptic technique. No specific physical findings were identified at the time of the procedure. The patient stayed on bed rest in the supine position and slept in the same posture. The CT scan taken immediately after the EBP procedure demonstrated pneumocephalus in the prepontine and premedullar cisterns (Fig. 1A). After waking on the fifth postoperative day, the first postprocedure day following the EBP, she started to complain of an abrupt vision abnormality. Her vital signs were stable and no neurological symptoms were detected other than her visual disturbance, apart from her persistent mild headache. Visual field and fundal examinations were conducted in the Department of Ophthalmology. A right homonymous hemianopia was detected in the Humphrey visual field test (Fig. 2), but no abnormal findings were identified on fundal examination. Magnetic resonance imaging (MRI) was performed due to the clinical suspicion of homonymous hemianopsia, and demonstrated air bubble movement toward the left retrochiasmal visual pathways (Fig. 1B).
After pneumocephalus was identified as the cause of her visual disturbance and headache, we administered prophylactic antibiotics and highly concentrated oxygen. The patient was then placed on bed rest. Her symptoms of visual disturbance improved considerably over the course of the day, and a follow-up CT scan was performed. No further air density was observed. Although her mild headache remained, the visual disturbance completely disappeared by the end of the fifth postoperative day. The patient was discharged on the sixth postoperative day and was asymptomatic at her outpatient follow-up visit one week later.
A case of temporary homonymous hemianopsia due to pneumocephalus after EBP has not been previously reported. Pneumocephalus is one of the potential complications in procedures that may result in dural puncture and is often reported after unexpected dural puncture, spinal anesthesia, or medication injection into the spinal canal during epidural anesthesia. Although it is very rare, a few cases of pneumocephalus have been reported after EBP for PDPH treatment, similar to this case report. Silvia et al. reported a case of hemipupillary dilatation associated with PDPH with evidence of pneumocephalus on CT scan. However, no previous studies have reported the unique constellations of symptoms including homonymous hemianopsia [4-8].
The LOR technique is commonly applied to identify the epidural space using either air or a physiological saline solution. The LOR technique with air can better detect the LOR than that using saline solution and enables more accurate and convenient verification of cerebrospinal fluid in cases of dural puncture. In addition, when saline is used, the identification of cerebrospinal fluid is more complicated, and local anesthetic agents may be diluted in the case of dural puncture. However, the use of air in this procedure brings with it the risks of pneumocephalus, aeroembolism, subcutaneous emphysema, and an uneven degree of sensory deprivation. These complications are nonetheless very rare, and air is more widely used because of the superior performance and convenience [4]. Pneumocephalus after the EBP procedure is assumed to occur due to the movement of air bubbles from the epidural space to subdural and subarachnoid spaces through the defect formed during the dural puncture [4]. Peumocephalus may also be generated by the movement of the remaining air in epidural space during dural puncture while performing the LOR technique or to remaining air in the subarachnoid space during dural puncture with additional air inflow during the EBP procedure [9]. Negative pressure induced by the inhalation of the patient during the procedure could also reduce cerebrospinal fluid pressure lower than atmospheric pressure. This is thought to be another potential mechanism of pneumocephalus [6,7,10].
Although not always simple, pneumocephalus and PDPH following a dural puncture can be distinguished by differences in clinical presentation. PDPH usually appears within one to four days of the dural puncture and persists for an average of four days; it is characterized by alleviation of headache in the supine position [4]. In comparison, the headache associated with pneumocephalus commonly appears immediately after the surgical procedure. Since the headache is generated by cerebral stimulation by the air present in the skull, the condition deteriorates despite any postural changes and continues even in the supine position [5].
In this case, the patient had symptoms consistent with PDPH, but the possibility of preoperative pneumocephalus could not be completely excluded. The comparison of pre- and post-operative images were unattainable since CT scanning was performed after the EBP procedure in this case report. However, symptoms prior to the EBP included only the typical postural headache without any vision abnormality. On the other hand, abrupt visual disturbance did occur immediately after the surgical procedure with postural change from supine position to sitting position. In addition, the pneumocephalus detected within the cistern on the CT scan taken before the onset of the homonymous hemianopsia moved to behind the optic chiasm in the MRI scan taken the next day, once the visual changes had been noted. This clinical course is consistent with the absence of pneumocephalus before the EBP procedure.
Our hospital frequently performs EBP without CT scanning in the presence of symptoms suspicious for PDPH. Through the experience of this unusual case, the authors realized that leakage of cerebrospinal fluid and possibilities for other illnesses should be considered, and CT scanning should be performed even in the presence of the typical history and symptoms of PDPH. In addition, the use of physiological saline is much safer than air for identifying the epidural space using the LOR technique, and the use of air needs to be carefully considered, especially after an unexpected dural puncture. In cases of air use according to the preference of anesthesiologist, the amount of air and the durations of syringe and guide needle use need to be reduced to minimize the air inflow to the epidural space.
References
1. Kattah JC, Dennis P, Kolsky MP, Schellinger D, Cohan SL. Computed tomography in patients with homonymous visual field defects: a clinico-radiologic correlation. Comput Tomogr 1981;5:301-312. PMID: 7326919.


2. Zhang X, Kedar S, Lynn MJ, Newman NJ, Biousse V. Homonymous hemianopias: clinical-anatomic correlations in 904 cases. Neurology 2006;66:906-910. PMID: 16567710.


3. Trobe JD, Lorber ML, Schlezinger NS. Isolated homonymous hemianopia: a review of 104 cases. Arch Ophthalmol 1973;89:377-381. PMID: 4697213.


4. Lee SS, Lee SG, Min BW, Ban JS, Lee JH, Kim EJ. Pneumocephalus after an autologous blood patch procedure to treat a postdural puncture headache. Korean J Anesthesiol 2008;55:387-390.

5. Hurtado TR, Clarkson FA. Pneumocephalus secondary to an epidural blood patch. Am J Emerg Med 2007;25:244-246. PMID: 17276839.


6. Kawamata T, Omote K, Matsumoto M, Toriyabe M, Ito T, Namiki A. Pneumocephalus following an epidural blood patch. Acta Anaesthesiol Scand 2003;47:907-909. PMID: 12859316.


7. Becker WJ. Pneumocephalus as a cause for headache. Can J Neurol Sci 2002;29:278-281. PMID: 12195619.


8. Laviola S, Kirvela M, Spoto MR, Tschuor S, Alon E. Pneumocephalus with intense headache and unilateral pupillary dilatation after accidental dural puncture during epidural anesthesia for cesarean section. Anesth Analg 1999;88:582-583. PMID: 10072010.


9. Lee KS, Kim YS, Lim JA, Kang PS, Lee YC. Effect of epidural autologous blood patch on the prevention of post-dural puncture headache after spinal anesthesia. Korean J Anesthesiol 1998;35:933-938.

10. Vasdev GM, Chantigian RC. Pneumocephalus following the treatment of a postdural puncture headache with an epidural saline infusion. J Clin Anesth 1994;6:508-511. PMID: 7880516.


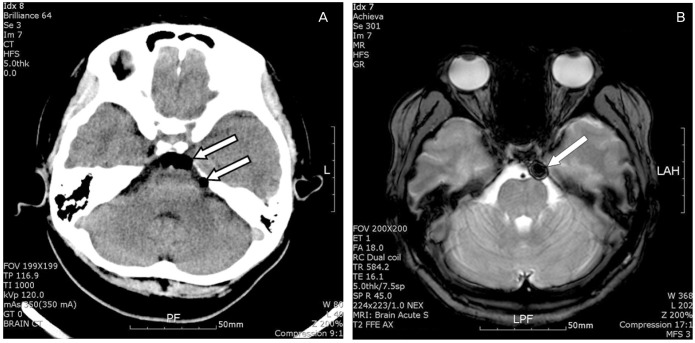
Fig.┬Ā1
(A) Computed tomography just after the epidural blood patch procedure demonstrates a small amount of pneumocephalus at the prepontine and premedullar cisterns (arrows). Visual disturbance had not yet developed. (B) T2-weighted fast field echo imaging demonstrates a small amount of pneumocephalus in the left retrochiasmal region (arrow) while the patient was complaining of visual disturbance.
-
METRICS

-
- 4 Crossref
- 3,550 View
- 43 Download
- Related articles in Obstet Gynecol Sci